Menu
Study
Ako
Life
Te Ao o UC
Contact us
Regular hours
Refer below for contact hours.
Special hours
The rehabilitation clinics at the Rose Centre is an evaluation and treatment clinic that offers specific, effective and innovative diagnostic and rehabilitative procedures for swallowing disorders (dysphagia) that are driven by the latest research and physiologic needs of our patients.
-
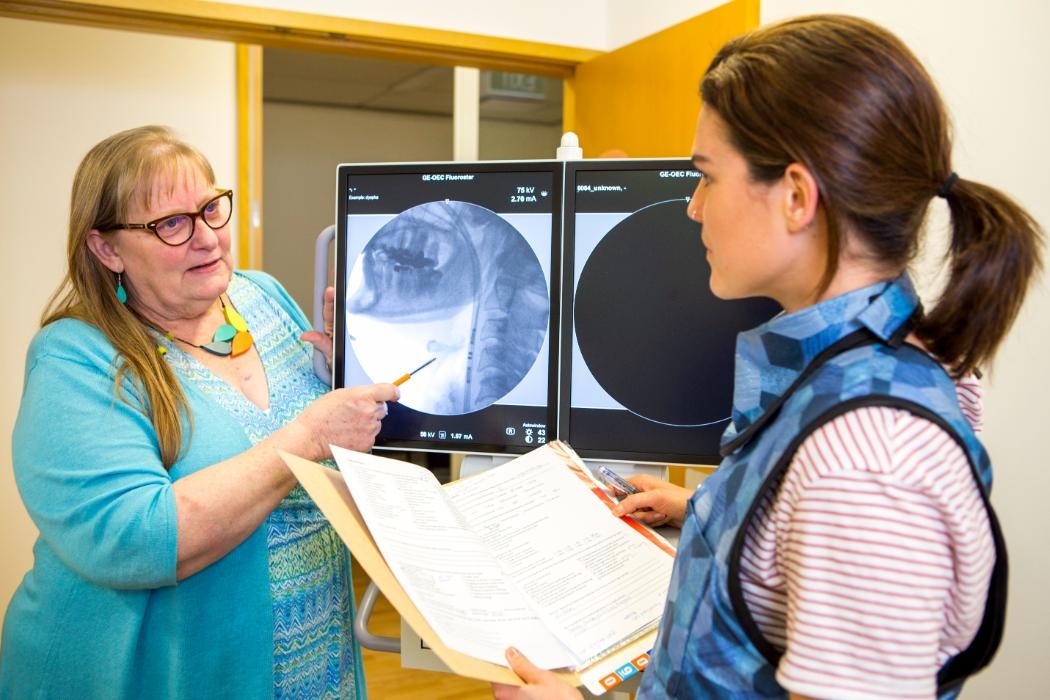
Rose Clinics - evaluation services
From swallowing to communication, learn about evaluation services at the Rose Clinics.
-
Rose Clinics - evaluation services
From swallowing to communication, learn about evaluation services at the Rose Clinics.

-

Rose Clinics - evaluation services
-
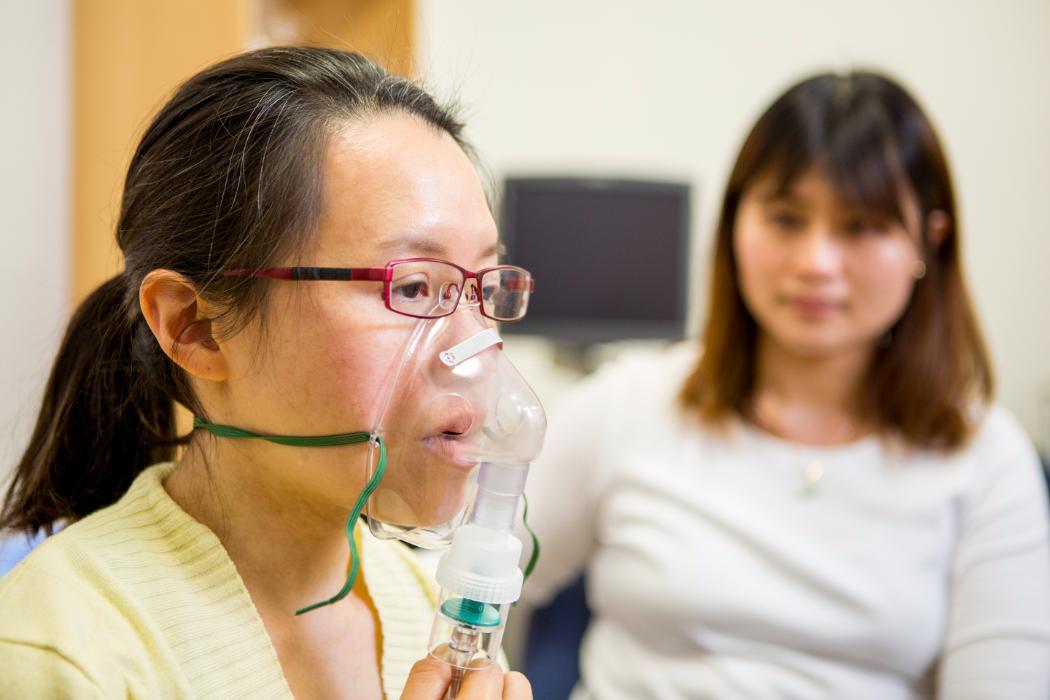
Treatment services
From dysphagia (swallowing difficulties) and aphasia (acquired language impairment disorder) to motor speech therapy, find out about treatment services at our Rose Clinics.
-
Treatment services
From dysphagia (swallowing difficulties) and aphasia (acquired language impairment disorder) to motor speech therapy, find out about treatment services at our Rose Clinics.

-

Treatment services
-
Rose Clinics fees
Our Rose Clinics assess and treat dysphagia, aphasia, and motor and speech difficulties. Find out about fees at our clinics.

-
Rose Clinics fees
Our Rose Clinics assess and treat dysphagia, aphasia, and motor and speech difficulties. Find out about fees at our clinics.

-

Rose Clinics fees
-
Referral to Rose Clinics
The Rehabilitation Clinics at the Rose Centre accept referrals from individuals, GPs, and therapists for assessment and rehabilitation. Find out about getting referred to our Rose Clinics.

-
Referral to Rose Clinics
The Rehabilitation Clinics at the Rose Centre accept referrals from individuals, GPs, and therapists for assessment and rehabilitation. Find out about getting referred to our Rose Clinics.

-

Referral to Rose Clinics
-
The Rose Centre for Stroke Recovery and Research
Donate to extend research and clinical expertise to address all aspects of rehabilitation for people recovering from a stroke.

-
The Rose Centre for Stroke Recovery and Research
Donate to extend research and clinical expertise to address all aspects of rehabilitation for people recovering from a stroke.

-

The Rose Centre for Stroke Recovery and Research
Testimonials
I hadn’t spoken to my throat in all my 65-years
Our patients are central to guiding the research that we do. While we help them recover function, they help us design new approaches, strategies and technologies for use with subsequent patients.
So when our patients speak, we listen. We hope you will as well.
The videos below are a testament to their strength and their faith in recovery and our commitment to the potential for rehabilitation.
Tony
An engineer by profession, Tony provides great insights about the use of biotechnology in rehabilitation at the Rose Centre.
Eric
Eric gave an inspiring speech about his experiences at the Rose Centre opening ceremony.
Our people
Lucy Greig, Clinical Director
Lucy Greig, MSc BSLT, graduated from the University of Canterbury in Speech and Language Therapy in 2000. She completed her Masters in Science (speech science) at The University of Auckland in 2011, examining the changes in word-retrieval in healthy older adults. Lucy has worked as a clinician in the field of dysphagia and acquired communication disorders across a variety of healthcare settings, including acute neurological and neurosurgical, inpatient rehabilitation, outpatient clinics and in the community.
Dr Maggie-Lee Huckabee, Rose Centre Director
Maggie-Lee Huckabee, PhD practised for 13 years before the frustration of never knowing ‘the answers’ led her to an academic career. She is a Professor at University of Canterbury and the Director of the UC Rose Centre for Stroke Recovery and Research. She worked clinically for many years before pursuing a research career but remains invested in best practice for dysphagia diagnosis and rehabilitation through clinically focusesd research and clinical consultation with Ms Greig on Rose Centre patients.
Dr Phoebe Macrae, Rose Centre Deputy Director
Phoebe Macrae, PhD completed her doctorate under the supervision of Maggie-Lee Huckabee. She was awarded a two-year Neurological Foundation post-doctoral fellowship at Johns Hopkins University, investigating motor learning in swallowing and continuing work in swallowing neurophysiology. Phoebe has returned to Christchurch to continue her research in dysphagia rehabilitation.
Fiona Bellett, Rose Centre Administrator
Fiona is the smiling face of the Rose Centre, greeting our patients, encouraging the staff and managing the administration and paperwork. Previously, Fiona has worked as an administrator for the NZBRI and for law firms in the Christchurch region.
Centre staff
By clicking "Accept All Cookies", you agree to the storing of cookies on your device to enhance site navigation, analyse site usage, and assist in our marketing efforts.
General enquiries
0800 827 748 (within NZ)
+64 3 369 3999
Emergency contact details
Ext: 92111 (from a campus landline)
Direct dial: 0800 823 637
University of Canterbury | A Fair Trade University






